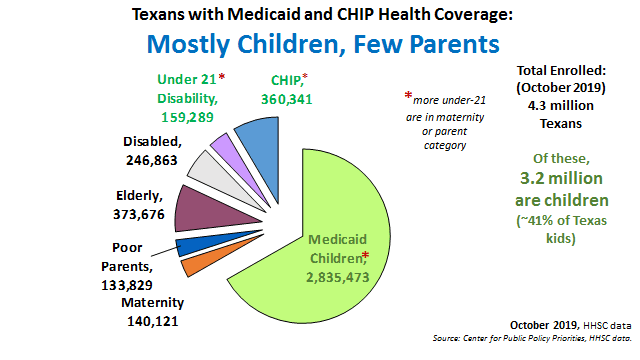
In 2019, about 4 million Texans were covered by Medicaid on any given day, about 3 million of them children. Texas has the lowest income limit for parents to get Medicaid in the U.S., so only a handful of the children on Medicaid have parents who qualify themselves.
Not everyone who is an uninsured U.S. citizen in poverty can get Medicaid in Texas, and coverage of non-U.S. citizens is limited, even for legal permanent residents.
- Very few parents can access Texas Medicaid; left out of Texas Medicaid are parents with incomes between 18% and 100% of the federal poverty income.
- Adults with serious, chronic, or mental illness. Disability-related Medicaid only becomes available when a person is no longer able to work at all, or is considered to be within 12 months of death. As a result, uninsured Texans with serious diagnoses struggle to continue working without adequate treatment.
- Uninsured Adults in Poverty. Texas Medicaid does not cover adults in poverty without dependent children, unless they have a serious or permanent disability, are elders in poverty, or get temporary maternity coverage that ends 2 months after the birth. The Affordable Care Act (ACA, or Obamacare) directed that all 50 states would offer Medicaid to US citizen adults, but a 2012 Supreme Court Decision ruled that states that did not provide that coverage could not be penalized with loss of federal Medicaid funds. As of May 2020, Texas was one of only 14 states not providing Medicaid to adults in poverty.
Many Texans are not aware that under federal law, ACA insurance subsidies are only available for U.S. citizens who are above the federal poverty income. This leaves most working-poor Texas adults uninsured, because our state’s Medicaid program is closed to them, and they cannot get sliding-scale ACA coverage either.
Texas qualifies for 90% federal funding for Medicaid expansion. A number of conservative states have coverage programs with co-pays, private insurance plans, and other market-based components.
A solution would benefit those Texans in the Coverage Gap and their families by ensuring they have access to cancer treatment, mental health care, preventive care that saves lives and money, and other care that is not available in the ER or in the patchwork of other services for the uninsured. It would also provide significant economic benefits, with the potential to create up to 230,000 jobs over three years, according to an estimate by former Deputy Texas Comptroller Billy Hamilton.