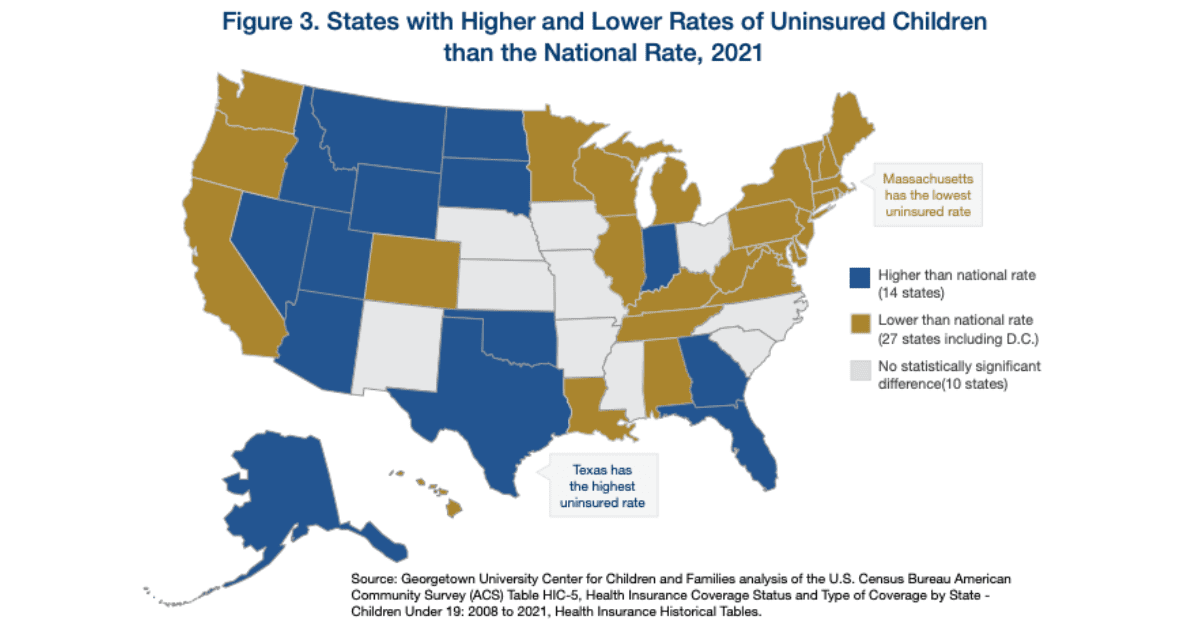
AUSTIN — A new report released today by the Georgetown University Center for Children and Families (CCF) shows that Texas had the nation’s worst uninsured rate for children in 2021. The report also shows that the uninsured rate for children declined nationally and in Texas thanks to Medicaid policies implemented during the pandemic Public Health Emergency (PHE).
Drawing on data from the Census Bureau’s American Community Survey, the report found that the number of uninsured Texas children fell from 995,000 in 2019 to 930,000 in 2021 as Texas and other states received federal funding under the PHE to allow children to remain enrolled in Medicaid without renewing their coverage. Texas’ children’s uninsured rate fell from 12.7% in 2019 to 11.8% in 2021 — a children’s uninsured rate that ranks 51st in the nation and is more than twice the national average of 5.4%.
“The improvement in the child uninsured rate has been a bright spot during the dark days of the pandemic,” said Joan Alker, executive director of the Georgetown University research center and lead author of the report. “This is welcome news for America’s children, but it may be short-lived as millions of eligible children will likely fall through the cracks and become uninsured in states that are inattentive when the federal continuous coverage protection expires.”
The PHE is expected to be in place until at least April 2023. The report warns that Texas and other states must prepare to effectively process Medicaid applications for children when the continuous coverage policies come to an end. Texas health groups have expressed concern that the state is not prepared.
“Some states do a better job than others in limiting red tape and modernizing their enrollment systems, which minimizes the risk of eligible children losing coverage,” said Alker. “States are primarily responsible for managing Medicaid and CHIP so the buck will stop with the Governor if children lose coverage. Congress could help protect children from unfairly losing coverage by establishing a minimum of 12 months of continuous eligibility for children in every state.”
“Kids make up three-quarters of Texas Medicaid and CHIP. How Texas leaders handle the “unwinding” of continuous coverage will overwhelmingly affect kids. If we mismanage this, we’ll see thousands of eligible kids kicked off their health insurance,” said Anne Dunkelberg, senior fellow at Every Texan. “We need all hands on deck to make sure Texas kids can see the doctor, get their medications, or go to their mental health appointments. We’re also very concerned that Texas leaders have decided to rush the renewal process, while other states have plans that will allow for a more orderly pace and accurate process for families when the Public Health Emergency ends.”
The report comes at a time when state legislators, including Texas House Speaker Dade Phelan, have called for action during the upcoming legislative session to ensure that eligible children are able to enroll in health coverage and renew their coverage.
“We’re so glad to see bipartisan momentum at the Legislature for improving outreach and access so eligible kids can have health insurance,” said Dunkelberg. “Texas must quickly address the delays, staffing shortages, and unintended barriers that Texans are already running into when they attempt to sign up for Medicaid or renew their coverage. State leaders could significantly improve our children’s uninsured rate — and make sure more kids get the health care they need — by making sure there’s an uncomplicated and efficient way for parents to get their kids covered.”
Advocates also called on state leaders to implement Medicaid expansion, a policy that would make parents and other adults with low incomes eligible for insurance through Medicaid. While the policy is directed at adults, the experience of other states shows that it reduces the children’s uninsured rate by helping parents connect with and navigate the Medicaid enrollment system. Texas is one of 11 states that has not adopted Medicaid expansion.